Side Effects | What are probiotics? | Sources of probiotics | Choosing a probiotic | Pre-biotics vs Probiotics | Alternatives to Antibiotics
Protect Your Gut Health While Taking Antibiotics
It can be tricky to untangle the root causes of digestive disorders as symptoms often overlap, allowing no specific diagnosis.
The problems may be linked to diet, stress, food intolerance or allergy, a gut infection, medication, or simply a change in routine.
However, excessive and inappropriate use of antibiotics may also be an underlying cause of many digestive issues.
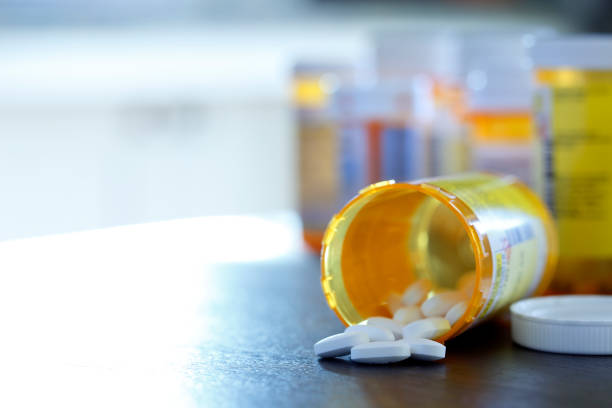
Antibiotics are undoubtedly one of the great advances in modern medicine, saving millions of lives every year.
(image credit: pccmarkets.com)
However, the over prescribed use of antibiotics within the medical industry, as well as in our food chain, is causing antibiotic resistance.
Furthermore, antibiotic resistance is developing faster than new antibiotics are being developed.
Some leading experts believe that there will be a serious health crisis in the future, with a total inability to treat some infectious diseases if we do not make more intelligent choices regarding antibiotics and use them less often.
According to the UK government: “It is estimated that at least 5,000 deaths are caused every year in England because antibiotics no longer work for some infections”.
Side Effects
A side effect of broad-based antibiotic drugs is that they are not very selective in choosing which bacteria to kill.
Antibiotics easily destroy friendly bacteria, which allows less healthy resident moulds, parasites, and yeasts such as Candida albicans to flourish and dominate in the gut.
Overgrowth of these pathogenic organisms is believed to be the root of many health complaints particularly as pathogens produce toxic substances, which are known to be harmful to the gut resulting in poor overall health.
Beneficial bacteria are so important for your health that it is imperative to restore the balance of gut flora after a round of antibiotic treatment by re-introducing the beneficial bacteria into the digestive process.
If this is ignored, there is an increased likelihood of developing ‘dysbiosis’ a disorder whereby there is an imbalance in the gut bacteria.
This commonly produces symptoms such as bloating, diarrhoea, constipation, wind, thrush and skin problems.
It could also contribute to health conditions such as diverticulitis, eczema, IBS and Crohns’ disease.
The importance of a well-balanced gut microbiome cannot be under-estimated when we think of the many processes, not just digestive, that rely on a balanced gut microbiome including weight control, cognitive health, and an increased risk of auto-immune diseases such inflammatory joint disease and allergies.
It is sensible to take a course of a multi-strain probiotic after a gut infection to calm down the irritated, inflamed tissues lining the bowel.
What are probiotics?
Probiotics are live non-pathogenic microorganisms that are beneficial to health if administered in adequate amounts.
They are tiny living organisms that can only be seen under a microscope and include: bacteria, viruses, and yeasts.
They make their way into your body via food, but can be introduced in a number of other ways including through the breath.
There are billions of bacteria and micro-organisms living in your body – your gastrointestinal tract alone is colonised by vast communities but they are also found on your skin and in your mouth.
The gut microflora is incredibly complex and dynamic and contains as many as 400 different species, which weigh around six pounds.
These microorganisms live symbiotically within you in a mutually beneficial relationship that has evolved to enhance their life and yours, protecting your health in a number of ways most importantly by processing nutrients and enhancing immune function.
Sources of probiotics
Probiotics can be found in yoghurt and many types of fermented foods such as:
- Miso
- Tempeh
- Sauerkraut
- Kimchi
- Kefir
- Soft cheeses like Gouda
- Sourdough bread
- Pickles
Choosing a probiotic
For a probiotic to be effective it needs to survive the digestive process.
Probiotic activity in foods like yoghurt can be compromised by the manufacturing process and transportation times – overly long shipment means once it reaches the consumer there may be little or no probiotic activity left.
There are also multiple strains and species of probiotics that have yet to be researched to prove whether or not they are effective.
It is important to choose a strain of probiotic that can establish itself and survive the harsh acidic environment and digestive juices of the stomach and intestinal tract.
Any health benefits conferred are generally specific to certain strains.
For example, Saccharomyces boulardi has been found to be effective in decreasing the duration of diarrhoea.
The difference between pre-biotics and probiotics
Compared with probiotics which introduce external bacteria into the colon, prebiotics are non-digestible carbohydrates that encourage the growth of a limited number of health-promoting or useful bacteria already living in the GI tract; especially but not exclusively Bifidobacterium and Lactobacillus. Combinations of probiotics and prebiotics are called ‘synbiotics’.
Some individuals don’t tolerate prebiotics very well and may experience digestive discomfort such as bloating and wind.
Starting with small amounts gives the gut time to adjust and may help to prevent any adverse symptoms.
Prebiotics can be found in the following foods:
- Chicory root
- Dandelion greens
- Jerusalem artichokes
- Bananas
- Oats
- Barley
- Asparagus
- Garlic
- Leeks
- Onions
- Wheat Bran
- Dietary supplements in the form of capsules, tablets, and powders
Natural alternatives to antibiotics
Why subject yourself to the adverse effects of antibiotics unnecessarily?
If you took advantage of the natural antimicrobials that grow all around us to treat minor infections such as coughs and sore throats, in many cases it wouldn’t be necessary to resort to antibiotic drugs at all.
Using natural antimicrobials and not over-using pharmaceutical antibiotics means they will be more effective when you really need them as in serious bacterial infections such as meningitis, sepsis, and pneumonia.
Mother Nature’s Medicine chest is abundant with healing plants that contain a range of anti-bacterial, anti-viral, anti-parasite and anti-fungal properties and if you can’t find them in your garden, they are freely available in supplement form in your local supermarket or health food shop.
Aloe Vera, garlic, cranberry, oregano, pelargonium, and echinacea are just a few of the amazing antimicrobials nature has to offer that can help combat anything from the common cold to gastrointestinal and urinary infections.
If you want to learn more about natural antibiotics you can read our blog: Nature’s own Antibiotics – A Natural Alternative.
If you’d like to comment on this article please feel free to fill in the form below.
We’d also like to hear about any successes you may have had with natural antibiotics or any that we may not have mentioned that you’d like to recommend.
Related Gut Health Topics:
- Gut Health – Common Gut Problems
- Gut Health – Is My Gut in Balance?
- Gut Health – Leaky Gut and Grains (and why to avoid them)
- Gut Health – The Gut at the Centre of your Health
- Gut Health – Good Health Starts in the Gut
- New Study Shows a Gluten Free Diet Influences Gut Health
- Gut Health – Fasting For Gut Health
- Gut Health – Antibiotics and Gut Health
- Control IBS With These 7 Foods
References
- Agoglu S and Alemander S. Investigation of In Vitro Antimicrobial Activity of Aloe Vera Juice. Journal of Animal and Vetinary Advances; 2009, 8 (1):99-102.
- Antibiotic resistance– the impact of intensive farming on human health A report for the Alliance to Save Our Antibiotics. [Accessed 27.7.18.]
- Billoo A, Memon M, Khaskheli S, et al. Role of a probiotic (Saccharomyces boulardii) in the management and prevention of diarrhoea. World Journal of Gastroenterology: WJG. 2006;12(28):4557-4560. doi:10.3748/wjg.v12.i28.4557.
- GOV.UK. Taking antibiotics when you don’t need them puts you at serious risk. [Accessed 4.8.18.]
- Kumar A & Upadhyaya R. Clinical Benefits of Manipulating the Gut Flora. Medicine Update 2008; 18, 257-63.
- Reagen K. Colorado State University. The 10 best food sources of prebiotics.[Accessed 2.8.18.]