Alzheimer’s disease is the most common form of dementia, affecting over 60% of the 850,000 dementia-sufferers in the UK.
It’s on the increase, with a projected 1 million sufferers by 2025. Put simply, researchers believe your lifetime risk of developing Alzheimer’s disease is now 15%.
We always take an evidence-based approach and in this article we will look at some factors which may predispose towards the development of the disease and suggest some strategies to reduce your Alzheimer’s risk.
Table of Contents:
- What are the symptoms?
- Treatment options
- Diet
- Stress
- Sleep
- Nutrition
- Exercise
- Brain stimulation
- Hormone balance
- Blood sugar balance
- Oral hygiene
- Fasting
What are the symptoms?
Symptoms of Alzheimer’s include memory loss, particularly for recently-learnt information, problems doing familiar tasks, losing track of dates and failure to recognise faces.
Before Alzheimer’s develops, sufferers experience Mild Cognitive Impairment (MCI), followed by Subjective Cognitive Impairment (SCI), when the decline in memory is noticed by the patient.
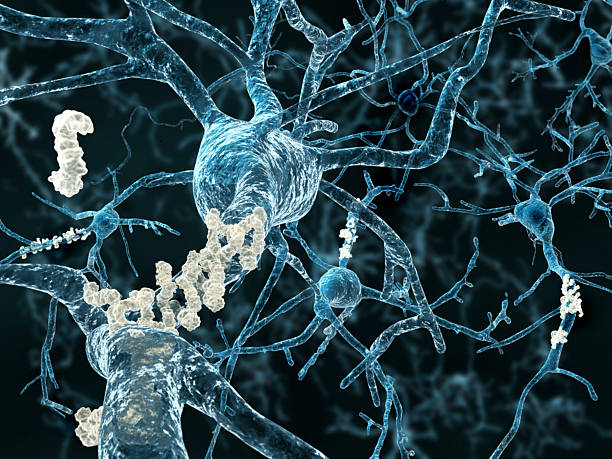
Although we don’t know a great deal about what actually causes Alzheimer’s disease, scientists have found substances called amyloid plaques in the brain of sufferers. Beta amyloid is a fragment of a protein naturally produced by the body.
It’s usually found in a brain cell’s fatty nerve sheath – normally the protein fragments would be eliminated from the body.
But in Alzheimer’s they accumulate forming hard, insoluble plaques which interfere with brain functioning, particularly with the functioning of synapses. A synapse allows a nerve cell to pass an electrical impulse to another cell – in other words, to communicate with it.
There appears to be a genetic risk for developing Alzheimer’s. There are three types of Apolipoprotein (APOE) gene and all have similar functions, to do with carrying fats, cholesterol and vitamins around the body and into the brain.
They also help clear the body of beta amyloid. We all have two copies of the gene, and the combination determines your ApoE genotype.
ApoE2 appears to be protective against Alzheimer’s, and scientists don’t yet know the effects of ApoE3.
However, people possessing the genotype ApoE4 have the strongest genetic Alzheimer’s risk, and more likelihood of developing it at a younger age.
People with the ApoE4 genotype appear to be predisposed to forming amyloid plaques.
They also seem to be more at risk of forming another type of protein called Tau.
Normally, Tau forms part of the microtubule of our cells, which transports nutrients from one part of a cell to another.
However, in Alzheimer’s, Tau is instead found in twisted fibres in brain cells known as Tau tangles or neurofibrillary tangles.
These tangles are found particularly in the areas of the brain associated with cognitive function.
Inflammation also appears to play a role.
Scientists think that special cells called microglia, whose role is to break down amyloid plaques and Tau tangles, may be put on high alert by the immune system and end up destroying healthy brain cells.
Currently, no medical protocol exists to treat Alzheimer’s with any success.
The only drugs in use can lessen symptoms for a limited period, but no medicine can reverse damage to the nerve cells which has already occurred.
Treatment options
What is clear is that there are multiple factors in the development of Alzheimer’s and a number of mechanisms involved.
It’s been suggested by scientists at the University of Southern California that as many as one in three cases are attributable to diet and lifestyle factors.
Recent research investigated a diet called the MIND diet.
This diet incorporates elements of the DASH (Dietary Approaches to Stop Hypertension) diet as well as the Mediterranean Diet. MIND stands for ‘Mediterranean-DASH Intervention for Neurodegenerative Delay’, and it’s been found to reduce Alzheimer’s risk by an incredible 53%.
Recently, a ground-breaking study using a personalised diet and lifestyle programme, dubbed ‘Metabolic Enhancement for Neurodegeneration’ or MEND, and further expanded on by Dr Dale Bredesen into the Bredesen Protocol, observed a reversal of the cognitive decline seen in the early stages of Alzheimer’s – something that previously, researchers believed was impossible.
In the study, researchers tracked participants, who were older adults with Alzheimer’s, MCI or SCI for 4-5 years and found those who followed the protocol had brains as if they were an average of more than seven years younger than they actually were. Many were able to return to work or showed improved performance at work. One patient with MCI had an increase in hippocampal volume of 11.7%.
The hippocampus plays a role in our memory for life events and is part of our spatial memory system – our recall of where things are in space and time. Alzheimer’s patients have been found to have smaller hippocampal volumes.
In some cases, sufferers had experienced a decline over a period of years, so the reversal was remarkable. It appeared that as long as they stayed on the programme, patients did not suffer from any further cognitive decline.
The following are some practical suggestions drawn from the MEND protocol.
1. Diet
The principles of the MIND diet include emphasising green leafy vegetables and berries, non-farmed fish, beans and nuts, and reducing red meat, grains (especially gluten containing grains), pastries, fried and processed food, dairy and sugar. It encourages the use of olive oil. The aim of the diet is to reduce inflammation and decrease insulin resistance, while delivering a good range of nutrients needed by brain cells.
2. Stress
A study by researchers at the University of Sweden found stress in middle age can be related to Alzheimer’s in later life – in mice, at least. The stressed animals didn’t remember as well and had more beta amyloid in their brains.
Another study on humans followed women for 35 years and asked them about their stress levels at 16-year intervals.
The researchers discovered the risk of developing Alzheimer’s was 65% higher in women who reported repeated periods of stress in middle age. Stress can even reduce the volume of our hippocampus, and this has been seen as early as the third day of stress. Find out how to manage stress with yoga and meditation.
3. Sleep
Melatonin, a hormone which is produced in the brain to help us fall asleep, appears to be especially low in sufferers. In fact, poor sleep in itself may increase Alzheimer’s risk, as not getting enough sleep has been found to increase the amount of beta amyloid in the brain. This effect can be seen after just one night of disturbed sleep.
It appears that beta amyloid may be cleared by the body during sleep. Adopting strategies to improve sleep, such as meditation, caffeine avoidance and banning TV and digital gadgets from your bedroom, can help you to nod off.
4. Nutrition
Alzheimer’s sufferers have been found to have lower levels of Vitamin B12 and Vitamin D3. Fish oil, which contains anti-inflammatory omega-3 oils, so important for brain cell functioning, is also recommended. Coenzyme Q10 acts as an antioxidant. Supplementation of these nutrients has been found in numerous studies to be beneficial.
5. Exercise
Exercise increases blood flow and has been found to increase hippocampal volume by as much as 2%. It can also improve neurogenesis, the process by which new brain cells are generated, according to a study in the Journal of American Geriatric Society.
The WHO recommends everyone over 65 years of age should exercise for a minimum of 75 minutes vigorous exercise, or 150 minutes moderate exercise, per week, although research suggests energetic aerobic exercise has the best results. Try exercising vigorously – in other words, exercise that makes you out of breath – for around 30 minutes 3 days per week.
6. Brain stimulation
It makes sense that training your brain keeps it active and scientists think it may even build reserves of healthy brain cells, while also maintaining the connections between brain cells. However, research in this area has been mixed.
A study published by the American Heart Association found speaking at least two languages protected against cognitive impairment following a stroke.
Another study, this time by the University of South Florida, showed that over ten years, a type of brain exercise known as ‘speed of processing training’ significantly reduced the risk of dementia. However, there are so many other factors that could have been at play over those ten years, that more research is needed on this subject.
Dementia Australia recommends activities such as language learning, sudoku or playing an instrument.
7. Hormone balance
Research suggests the changes in oestrogen levels which occur as we get older may partly account for Alzheimer’s development.
Oestrogen is important for brain function. There are receptors for oestrogen in the brain, mainly in the hippocampus, where it seems to help the growth and survival of brain cells as well as having a role in amyloid metabolism, the productions of certain types of neurotransmitters and protecting the brain from the effects of inflammation.
Progesterone, on the other hand, appears to help brain cells to survive longer, as well as acting as an anti-inflammatory.
Women who suffer from hormonal imbalance before the menopause, experiencing symptoms like PMS or infertility, seem to have a higher risk for Alzheimer’s once they reach the menopause.
After the menopause, women produce oestrogen from the adrenal glands and the liver, while men produce oestrogen by converting it from testosterone.
So if your liver is struggling or if your adrenals have been affected by long-term stress, hormones may be pushed out of balance.
Remember also that sex hormones are produced from cholesterol, so if cholesterol is too low, your sex hormones will inevitably be out of kilter.
Some success has been seen after using HRT, but results have been mixed, probably because synthetic progesterone was used, which does not work in the body in the same way as bio-identical progesterone.
It makes sense, however to adopt strategies to balance your hormones.
8. Blood sugar balance
Scientists have also found that people with Alzheimer’s have reduced glucose utilisation by the brain cells – in other words, they aren’t able to take on board sugar for energy as well as normal brain cells can.
There are insulin receptors in the brain, and in Alzheimer’s the brain cells appear to suffer from insulin resistance.
This seems to occur most markedly in the pariotemporal junction of the brain which collects information from our sense organs and is also involved in moral decisions.
Studies have found that Type 2 diabetes increases the risk of developing Alzheimer’s.
You’ll know from personal experience how sensitive the brain is to variations in blood sugar levels if you’ve ever experienced the jitters from going to too long without food.
Dietary strategies for balancing your blood sugar, such as avoiding caffeine, alcohol and sugar, may therefore reduce your Alzheimer’s risk.
9. Oral hygiene
Researchers have found the bacterium Porphyromonas gingivalis in brains of Alzheimer’s patients. This is normally found in the mouth in sufferers of gingivitis (gum disease) and it can easily pass into the bloodstream when gums bleed. It’s thought it may bring about an immune response in the brain which kills brain cells.
Make sure you brush your teeth properly, floss regularly and eat plenty of green, leafy vegetables, as well as fruit containing vitamin C which is vital for gum health. Avoid sugary foods and drinks, as well as fizzy soda drinks.
10. Fasting
During the MEND programme, patients were instructed to leave a minimum of twelve hours break between their evening meal and breakfast the next day, and at least 3 hours between their evening meal and bedtime.
Fasting in this way increases autophagy by the cells, particularly brain cells.
Autophagy is the body’s natural waste removal process, where old cells are removed and recycled in a neat housekeeping process and in this way inflammation in the brain can be controlled.
Although research is still ongoing and there is much still to be discovered about Alzheimer’s Disease, adopting the above strategies may help to keep your brain healthy.
We believe that sharing knowledge and experience is an important part of achieving optimal health.
We would love to hear from you, please get in touch.
Related Alzheimer’s Articles:
- Meditation reduces chances of Alzheimer’s
- Foods And Nutrients To Prevent Alzheimer’s Disease
- Green Tea – improves weight loss and memory too
Helpful Resources:
- Alzheimer’s and Dementia in the United Kingdom – www.alz.org
- Online learning resources for professionals – alzheimers.org.uk
- Alzheimer’s Research UK – alzheimersresearchuk.org
- NHS Dementia guide – www.nhs.uk
Charities for people with dementia
- National Dementia Helpline 0300 222 11 22
- Dementia UK 0800 888 6678
- Alzheimer’s Research UK 0300 111 5 111
- Age UK 0800 055 6112
Forum
References
Dementia prevention, intervention, and care, Gill Livingston, Andrew Sommerlad, et al . Volume 390, No. 10113, p2673–2734, 16 December 2017
Early hippocampal volume loss as a marker of eventual memory deficits caused by repeated stress, Mohammed Mostafizur Rahman et al, Scientific Reports volume 6, Article number: 29127 (2016)
Hippocampal volumes in Alzheimer’s disease, Parkinson’s disease with and without dementia, and in vascular dementia: An MRI study. Laakso MP, et al. Neurology. 1996.
Hormonal Influences on Cognition and Risk for Alzheimer Disease, Sarah C. Janicki, M.D., M.P.H and Nicole Schupf, Ph.D., Dr.P.H; Curr Neurol Neurosci Rep. 2010 Sep; 10(5): 359–366.
Formation and effects of neuroactive steroids in the central and peripheral nervous system. Melcai, R, et al. Int Rev Neurobiol 2001; 46: 145-76
Insulin Resistance and Alzheimer’s Disease: Bioenergetic Linkages. Bryan J. Neth and Suzanne Craft; Front Aging Neurosci. 2017; 9: 345.
Exploring the Association between Alzheimer’s Disease, Oral Health, Microbial Endocrinology and Nutrition, Alice Harding et al. Dementia & Neurodegenerative Diseases Research Group, Faculty of Clinical and Biomedical Sciences, School of Dentistry, University of Central Lancashire, Preston,
MIND diet slows cognitive decline with aging, Martha Clare Morris et al. Alzheimers Dement. 2015 Sep; 11(9): 1015–1022.
Amyloid accumulation in the human brain after one night of sleep deprivation. Shokri-Kojori E et al Proc Natl Acad Sci USA. 2018 Apr 9
Vitamin B12 levels in Alzheimer’s disease: association with clinical features and cytokine production. Politis A, et al. J Alzheimers Dis. 2010.
Vitamin D and the risk of dementia and Alzheimer disease. Thomas J. Littlejohns, et al. Neurology. 2014 Sep 2; 83(10): 920–928
Exercise training increases size of hippocampus and improves memory. Erickson KI, et al. Proc Natl Acad Sci U S A. 2011.
Short-term fasting induces profound neuronal autophagy. Alirezaei M, et al. Autophagy. 2010.